 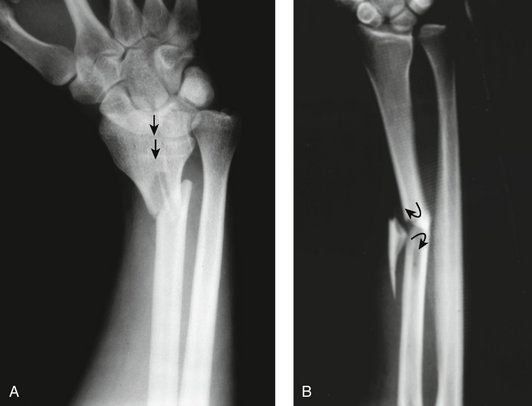
The great majority of distal radius fractures are closed fractures, where the overlying skin and tissues are intact. There is often deformity in the case of displaced fractures and movement restriction can result. These are unstable fractures.Ī distal radius fracture is painful, with local tenderness and swelling. These are unstable fractures and, like buckle fractures, occur in younger children ( Randsborg 2009).Ĭomplete metaphyseal fractures are fractures across the bone where both sides of the cortex are disrupted if displaced, the fractured end fragment is usually displaced dorsally relative to the rest of the bone. However, variation in the definition of where distal forearm fractures start can mean that shaft fractures are also included. This fracture pattern occurs predominantly in the shaft and, strictly speaking, greenstick fractures are not metaphyseal fractures. Greenstick fractures are where the bone is broken on one side but only bent (compressed) on the opposite side. They are by far the most common distal radius fracture ( Randsborg 2012 Thimmaiah 2012). Buckle fractures are considered stable fractures, with little risk of subsequent deformity ( Macnicol 2010 Randsborg 2012 Slongo 2007). This results in a deformity but not a complete break in the cortex. These 'metaphyseal' fractures occur in the metaphysis, the area that lies between the shaft (diaphysis) and the growth plate.īuckle or torus fractures involve compression of only part of the circumference of the cortex (outside part) of the bone. The other three categories of paediatric distal radius fractures commonly described in the literature are: 'buckle' or 'torus' fractures 'greenstick' fractures and complete or 'off‐ended' fractures. The most frequently used classification of physeal injuries is that of Salter and Harris ( Salter 1963). Growth‐plate fractures of the distal radius are more common in older children ( Mizuta 1987). Fractures involving the growth plate are called also physeal fractures. Growth plates are areas of cartilage near the end (epiphysis) of the long bones in children and adolescents. They vary in severity, complexity and location in relation to the growth plate (physis) and the age of the child. The distribution of fractures is unimodal for both sexes ( Rennie 2007) Hedström 2010 reported peaks at 11 years for girls and 14 years for boys.ĭistal radius fractures most commonly result from a fall on an outstretched hand. The mean age of children (aged up to 16 years) presenting with these injuries in 2000 at two Edinburgh hospitals was 9.9 years and 55% were boys ( Rennie 2007). Annual incidences of 30 per 10,000 children (aged 0 to 17 years) have been reported in the US during 2009 ( Karl 2015). Isolated distal ulna fractures are rare and not considered further here.ĭistal radius fractures are the most common fractures in children, amounting to around a quarter to a third of all paediatric fractures ( Hedström 2010). Sometimes they can be accompanied by an adjacent fracture of the ulna. Most fractures involve the distal radius, which is the focus of this review. Wrist fracture is often used to describe breaks in the distal parts (roughly the distal third) of these bones. The two forearm bones are the radius and the ulna. The Management of Isolated Distal Radius Fractures in Children. 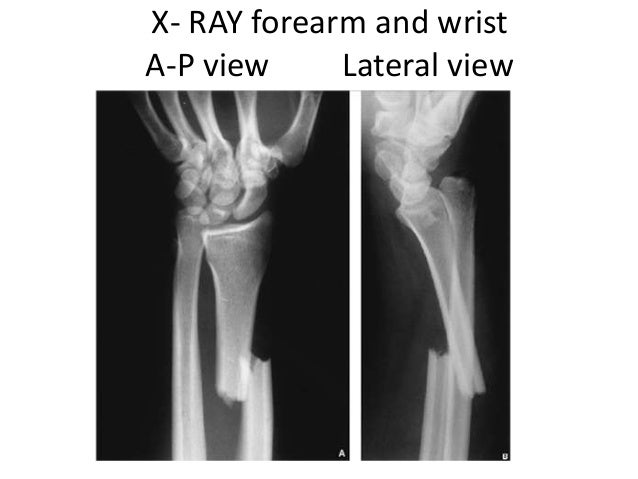
Īngular remodeling of midshaft forearm fractures in children. Galeazzi-equivalent injuries of the wrist in children. Variant of Galeazzi fracture-dislocation in children. in child over 12 yrs, if reduction is not acceptable, then treatment is ORIF of radius w/ 4 hole plate & closed reduction of distal RU joint w/ radius out to length the distal RU joint is reduced and held in full supination in a long arm cast for 6 weeks if closed reduction is still not possible, then insert a 1 mm K wire percutaneously into fracture site and use it "lever" the fracture into a reduced position in this situation, the child should receive general anesthesia and undergo repeated closed reduction although in the past, bayonet position was accepted in children younger than 8 years, this is no longer the standard of care in some cases, anatomic reduction may not be possible with simple closed reduction difficult reduction may be due to entrapment of pronator quadratus over the proximal fragment closed reduction w/ longitudinal traction, & correction of radial angulation due to the significant force needed for reduction, consider GEA frx is usually displaced dorsally and shortened in bayonette position
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
